What Does Medicare Not Cover? Eight Things You Should Know
Medicare Part A and Part B leave gaps in your healthcare coverage. But Medicare Advantage has problems, too.


Medicare Part A and Part B, also known as original Medicare or traditional Medicare, cover a large portion of your medical expenses after you turn 65, but that doesn't mean Medicare covers everything.
Part A (hospital insurance) helps pay for inpatient hospital stays, skilled nursing facility stays, surgery, hospice care and even some home health care. Part B (medical insurance) helps pay for doctors' visits, outpatient care, some preventive services, and some medical equipment and supplies. Most people can start signing up for Medicare three months before the month they turn 65.
It's important to understand that Medicare Part A and Part B leave some pretty significant gaps in your health care coverage; many buy Medigap policies to pick up those costs. This is why an increasing number of Medicare beneficiaries choose a Medicare Advantage plan (MA) to fill some of those gaps. However, be aware that any extras or perks could be reduced or withdrawn in a later plan year.
From just $107.88 $24.99 for Kiplinger Personal Finance
Become a smarter, better informed investor. Subscribe from just $107.88 $24.99, plus get up to 4 Special Issues

Sign up for Kiplinger’s Free Newsletters
Profit and prosper with the best of expert advice on investing, taxes, retirement, personal finance and more - straight to your e-mail.
Profit and prosper with the best of expert advice - straight to your e-mail.
A private plan through Medicare Advantage, which customers generally like, can offer more benefits and lower premiums. But a 2022 report from the Office of Inspector General found that some beneficiaries of Medicare Advantage are denied necessary care.
Here's a closer look at what isn't covered by traditional Medicare, plus information about supplemental insurance policies, Medicare Advantage, and strategies that can help cover the additional costs, so you don't end up with unexpected medical bills in retirement.

1. Does Medicare cover prescription drugs?
Medicare doesn’t provide coverage for outpatient prescription drugs, but you can buy a separate Part D prescription drug policy that does, or a Medicare Advantage plan that covers both medical and drug costs. (Some retiree health-care policies cover prescription drugs, too).
You can sign up for Part D or Medicare Advantage coverage when you enroll in Medicare or when you lose other drug coverage. You can also change policies during open enrollment season each fall. Compare costs and coverage for your specific medications under either a Part D or Medicare Advantage plan by using the Medicare Plan Finder.
Married couples can pick different Part D policies and select the one that best covers their individual healthcare needs.
If you enroll in a Part D or Medicare Advantage plan for 2026, you won’t have to pay more than $2,100 in out-of-pocket costs for your medications. You will also have the option to spread out-of-pocket costs over the year rather than having to pay high out-of-pocket costs in any given month.
If you are enrolled in the Medicare Prescription Payment Program (MPPP) in 2026, you will be auto-enrolled for the next year unless you formally withdraw.
This cap on prescription drug costs applies only to medications covered by your Part D plan and does not apply to out-of-pocket spending on Medicare Part B drugs. Part B drugs include vaccinations, injections a doctor administers and some outpatient prescription drugs.
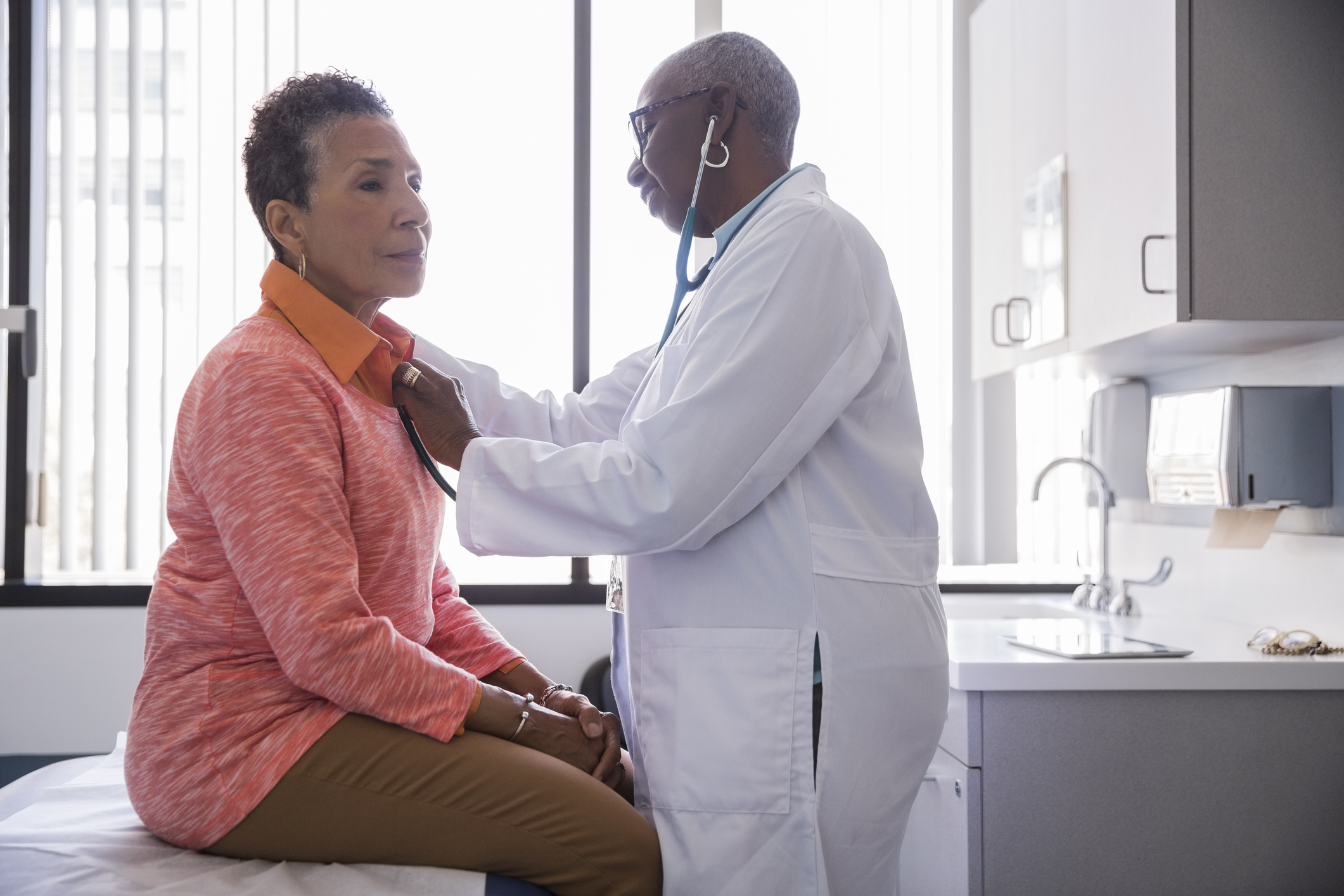
2. Routine physical exams
Annual physicals are not covered by Medicare. That may seem short-sighted, as annual physicals have typically been recommended as a preventative measure to head off bigger medical issues with early detection. Medicare does cover a Medicare Wellness Visit, also called a wellness exam. This type of visit is an assessment of your overall health and well-being.
Medicare Part B covers an annual wellness exam and many preventive screenings with no copay or deductible. However, you may have to pay a share of the cost for certain recommended tests or services. And while it’s not mandatory, there are very good reasons to have a wellness exam every year.
During the exam, your primary care provider combines information from the visit with your medical record to assess your risk for common preventable health problems such as heart disease, cancer and type 2 diabetes. Based on what’s learned from your exam, your doctor will create a personal prevention plan with a checklist of screenings you need to have.
Medicare covers a wellness visit once every 12 months (11 full months must have passed since your last visit), and you are eligible for this benefit after you have had Part B for at least 12 months.

3. Does Medicare cover long-term care?
One of the largest potential expenses in retirement is the cost of long-term care. The median cost of a private room in a nursing home was roughly $135,528 in 2026 (according to Genworth estimates cited by SeniorLiving.org); a room in an assisted-living facility costs $75,756, and a home health aide costs $200 per day.
Medicare provides coverage for some skilled nursing services but not for custodial care, such as help with bathing, dressing and other activities of daily living. However, you can buy long-term-care insurance or a combination long-term-care and life insurance policy to cover these costs.
You can also get a long-term care rider on an annuity, which can help defray the cost of long-term care.

4. Does Medicare cover deductibles and co-pays?
Medicare Part A covers hospital stays, and Part B covers doctors’ services and outpatient care. But you’re responsible for deductibles and co-payments.
In 2026, you’ll have to pay a Part A deductible of $1,736 before coverage kicks in, and you’ll also have to pay a portion of the cost of long hospital stays — $434 per day for days 61-90 in the hospital and $868 per day after that.
Be aware: Over your lifetime, Medicare will only help pay for a total of 60 days beyond the 90-day limit, called “lifetime reserve days,” and thereafter you’ll pay the full hospital cost.
Part B typically covers 80% of doctors’ services, lab tests and x-rays, but you’ll have to pay 20% of the costs after a $283 deductible in 2026. A Medigap (Medicare supplement) policy or Medicare Advantage plan can fill in the gaps if you don’t have the supplemental coverage from a retiree health insurance policy. Medigap policies, sold by private companies, come in 10 standard versions that pay for costs that original Medicare doesn't cover.
If you buy a Medigap policy within the first six months of signing up for Medicare Part B, insurers can’t reject you or charge more because of preexisting conditions. After your initial enrollment period, insurers can use underwriting to assess your fitness for a policy and adjust your premium. See Compare Medigap Plan Benefits at Medicare.gov for more information, as well as Watch Out for the 'Medigap Trap.'
Medicare Advantage plans provide medical and drug coverage through private insurers, and many also offer supplemental benefits for vision and dental care. You can switch Medicare Advantage plans every year during open enrollment season.
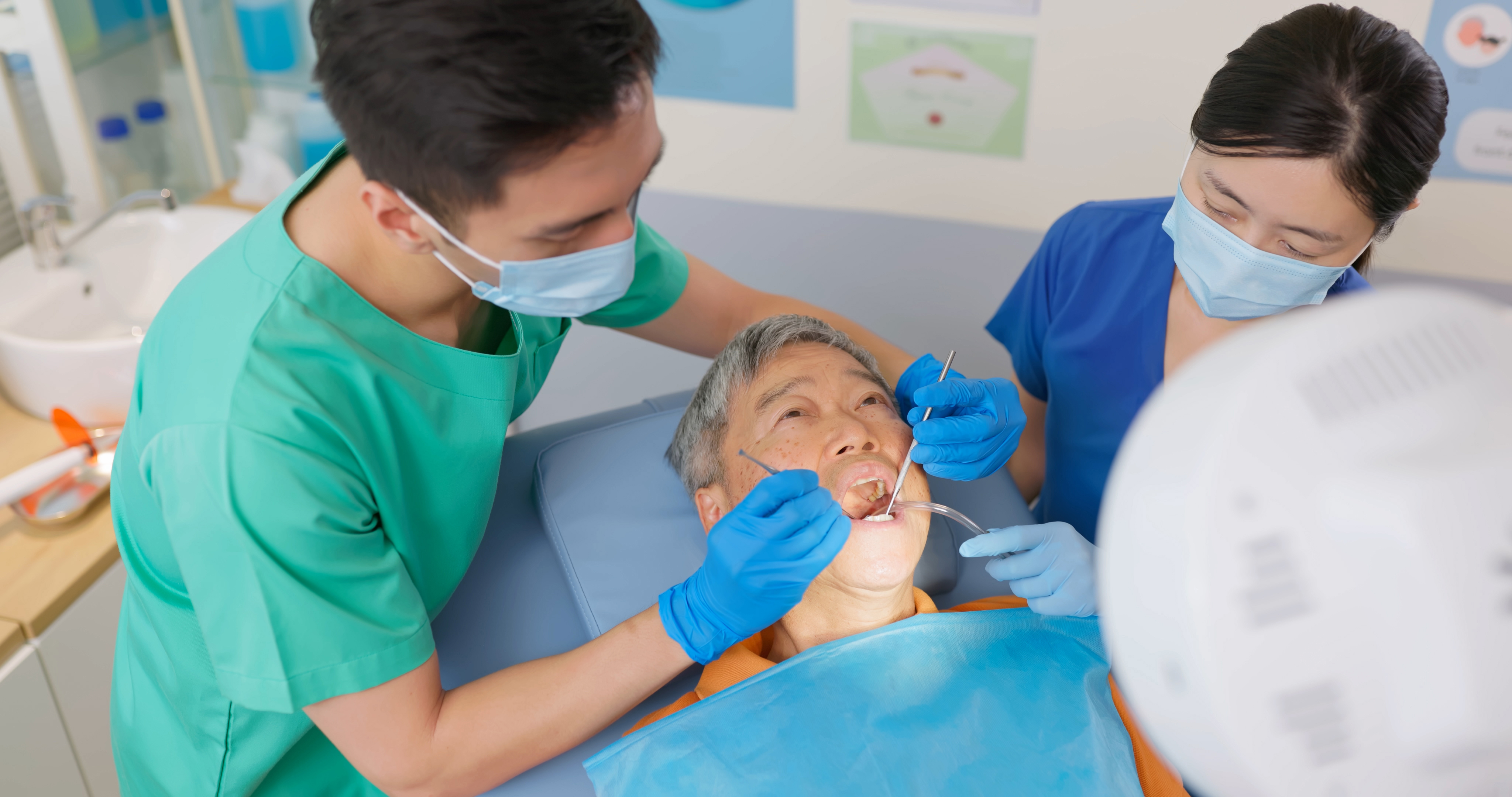
5. Does Medicare cover dental care?
Medicare doesn’t provide coverage for routine dental visits, teeth cleanings, fillings, dentures, or most tooth extractions. Some Medicare Advantage plans cover basic cleanings and X-rays, but they generally have an annual coverage cap of about $1,500. You could also get coverage from a separate dental insurance policy or a dental discount plan.
An alternative way to pay is to build up money in a health savings account (HSA) before you enroll in Medicare. You take tax-free distributions for medical, dental and other out-of-pocket costs at any age. However, you can’t make contributions to an HSA after you sign up for Medicare.
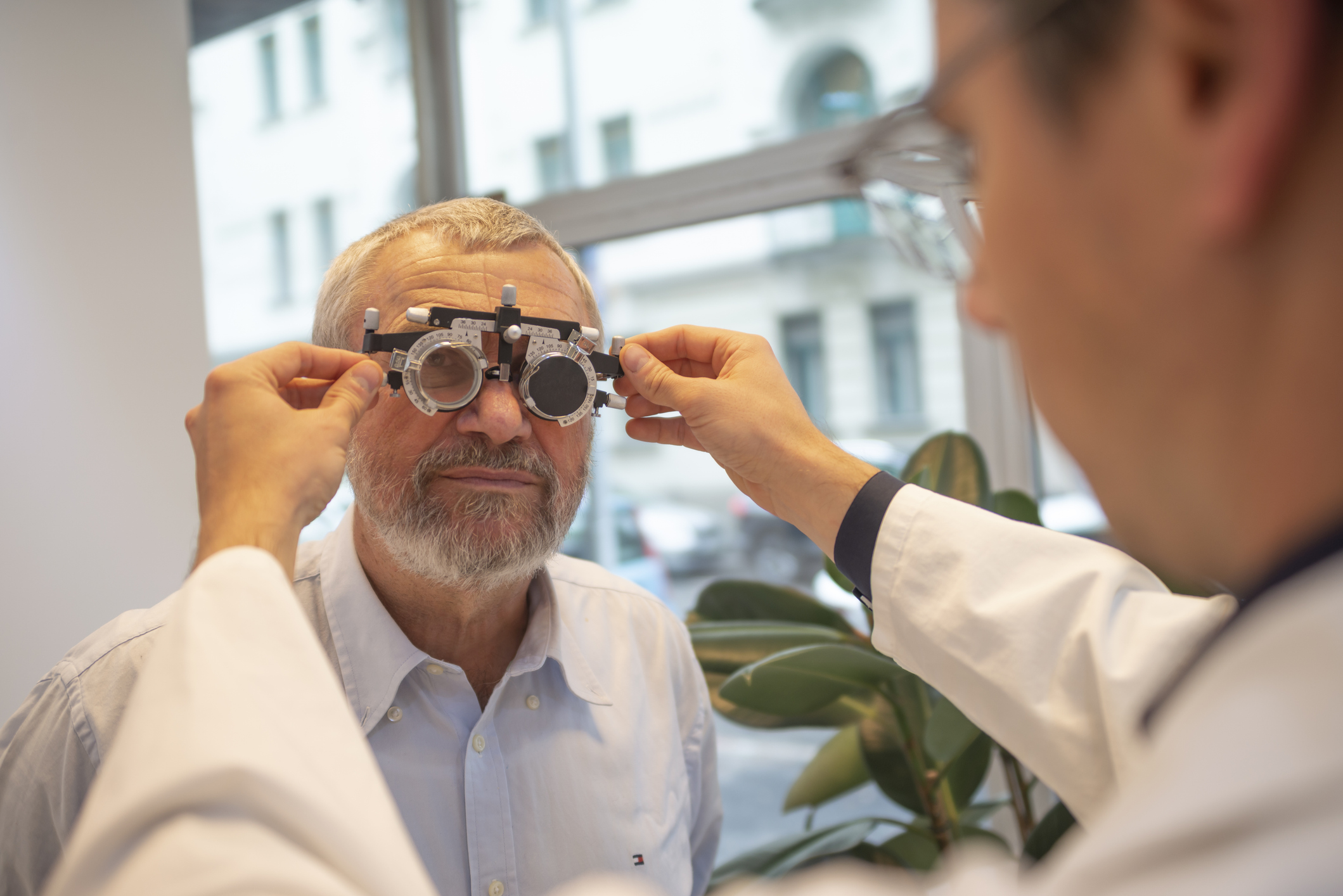
6. Does Medicare cover routine vision care?
Medicare generally doesn’t cover routine eye exams or glasses (exceptions include an annual eye exam if you have diabetes or eyeglasses after having certain kinds of cataract surgery). But some Medicare Advantage plans provide vision coverage, or you may be able to buy a separate supplemental policy that provides vision care.
If you set aside money in an HSA before you enroll in Medicare, you can take tax-free distributions at any age to reimburse yourself for exams, glasses, contact lenses, prescription sunglasses and other out-of-pocket costs for vision care.

7. Does Medicare cover hearing aids?
Hearing aids are critical for maintaining a healthy brain for those with hearing loss. A recent study found that hearing aids lowered the rate of cognitive decline in older adults at high risk of dementia by almost 50%.
Medicare doesn’t cover routine hearing exams or hearing aids, which can cost from $2,000 to $4,000 per ear. However, some Medicare Advantage plans cover hearing aids and fitting exams, and some discount programs provide lower-cost hearing aids. If you save money in an HSA before you enroll in Medicare, you can use the money tax-free for hearing aids, hearing tests, and other out-of-pocket expenses.
If you have mild hearing loss, an over-the-counter hearing aid might be a good fit for you. Senior Living says these devices typically cost between $99 and $8,000 a pair. Be sure to get an audiology test before you get over-the-counter hearing aids, as Johns Hopkins recommends.

8. Does Medicare cover medical care overseas?
Medicare usually doesn’t cover care you receive while traveling outside of the U.S., except for very limited circumstances (such as on a cruise ship within six hours of a U.S. port). But some Medigap plans will cover 80% of the cost of emergency care abroad up to a certain limit.
Medicare Supplement plans C, D, F, G, M and N cover some travel-abroad emergency help. No other Medicare Supplemental plans provide foreign travel emergency coverage.
Additionally, some Medicare Advantage plans cover emergency care abroad. Or you could buy a travel insurance policy that covers some medical expenses while you’re outside of the U.S. It may even cover emergency medical evacuation, which can otherwise cost tens of thousands of dollars to transport you aboard a medical plane or helicopter.

A note about Medicare Advantage
Medicare Advantage may provide coverage for some things not covered by traditional Medicare. However, as mentioned above, a 2022 report found that some Medicare Advantage insurance providers unnecessarily denied care or payments for care that would have been provided to beneficiaries had they chosen traditional Medicare.
The Advantage insurance providers likewise “denied payments to providers for some services that met both Medicare coverage rules” and the organizations’ billing rules, according to the report. This could prevent or delay needed care for beneficiaries and could result in a burden on medical providers.
The report also found that 13% of the time that Medicare Advantage providers denied prior authorization, the requests met rules making them eligible under original Medicare, suggesting they would have been approved if the beneficiaries had not chosen Advantage instead of original Medicare.
The report concluded that in those instances, Advantage insurance providers “used clinical criteria that are not contained in Medicare coverage rules.” For example, they might require an X-ray before approving more advanced imaging. In addition, the Advantage insurance providers denied some prior authorizations for care on the basis that the requests didn’t have enough documentation to support approval.
Yet, the inspector general found, “our reviewers found that the existing beneficiary medical records were sufficient to support the medical necessity of the services.”
Often, when challenged, however, the Advantage insurance providers would reverse their decisions. So, it’s important for patients to be able to advocate for necessary coverage if denied.
Lawmakers on both sides of the aisle introduced legislation in 2023 to curb frivolous denials of care by Advantage insurers. And the Department of Health and Human Services finalized rules in April 2024 to overhaul how Medicare Advantage customers get prior approval for care.
To look up Medicare’s coverage rules and other types of care and procedures, go to Medicare.gov/coverage and use the “Is my test, item or service covered?” tool. If you believe a claim was unfairly denied, see How to Appeal a Denied Medicare Claim.
Related content
Profit and prosper with the best of Kiplinger's advice on investing, taxes, retirement, personal finance and much more. Delivered daily. Enter your email in the box and click Sign Me Up.

Donna joined Kiplinger as a personal finance writer in 2023. She spent more than a decade as the contributing editor of J.K.Lasser's Your Income Tax Guide and edited state specific legal treatises at ALM Media. She has shared her expertise as a guest on Bloomberg, CNN, Fox, NPR, CNBC and many other media outlets around the nation. She is a graduate of Brooklyn Law School and the University at Buffalo.