You May Pay More for Your Prescription Drugs
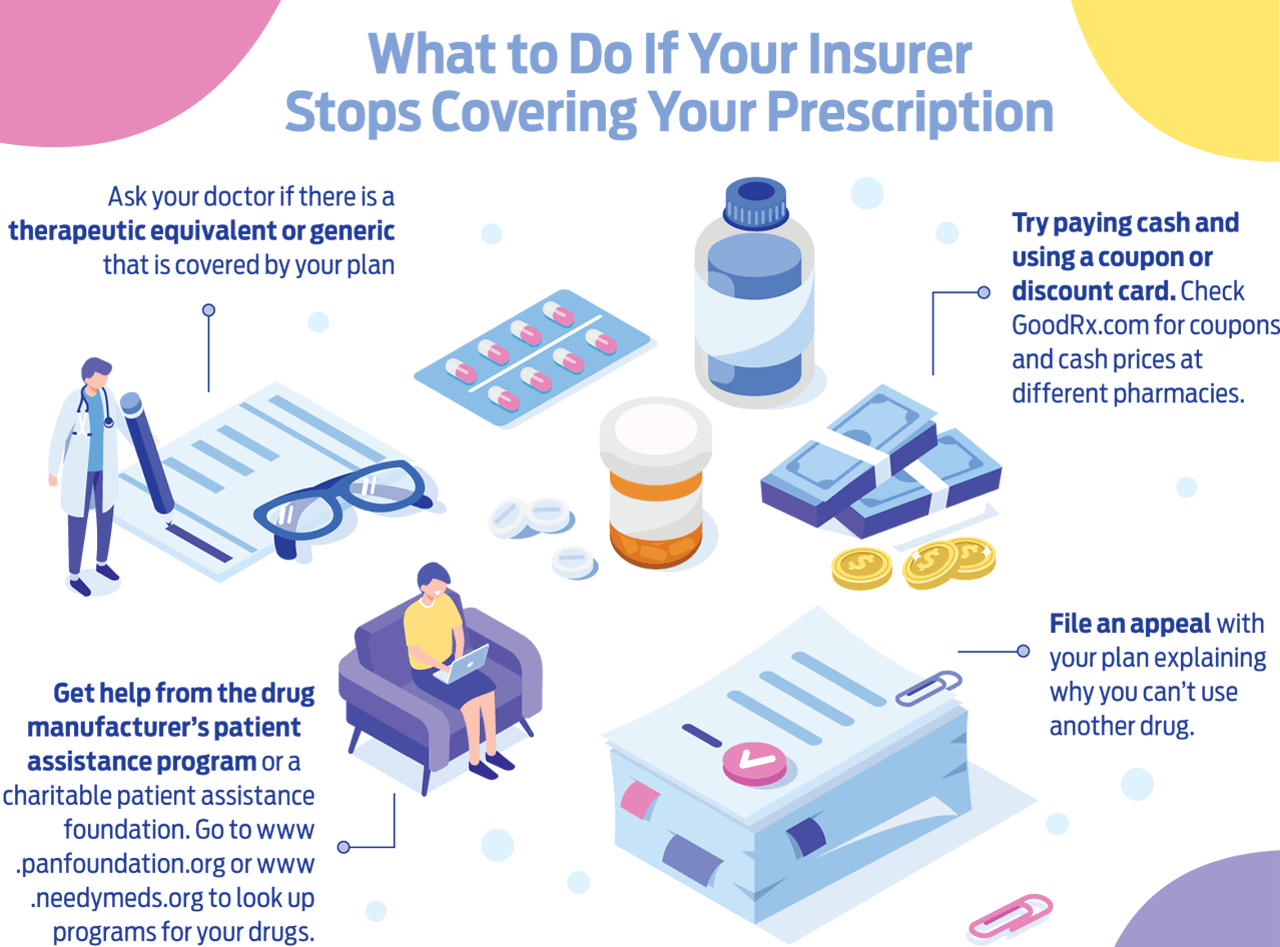
If your health insurance plan dropped your drugs from their formulary, you still have options.

If your insurance plan covers prescription drugs, you may be in for sticker shock the next time you go to the pharmacy. Express Scripts and CVS Caremark, two large pharmacy benefit managers that provide drug coverage for many health plans, dropped about 90 drugs from their preferred formularies (the list of drugs they cover) in 2019.
These changes can affect people who have coverage through their employer, as well as people who buy an individual policy. Specifics vary, but many insurers adopt the pharmacy benefit managers’ preferred formularies for their own coverage. (The drug lists can be different for Medicare Part D. The Trump administration has proposed new rules for Medicare plans that would require PBMs that receive rebates from drug companies to pass on the savings to consumers.)
If several drugs are deemed effective at treating a specific disease, the pharmacy benefit manager typically negotiates with drug manufacturers and chooses the option that costs it the least. That could cause a drug you’re using to be dropped from its formulary. If your drug is dropped, ask your doctor if you can switch to an alternative. For example, Pradaxa, a blood thinner that was dropped from Express Scripts’ formulary, costs about $500 for a 30-day supply without insurance. But you may be able to switch to warfarin, a generic version of a different blood thinner, which may be covered by your insurance with a small co-pay.
From just $107.88 $24.99 for Kiplinger Personal Finance
Become a smarter, better informed investor. Subscribe from just $107.88 $24.99, plus get up to 4 Special Issues

Sign up for Kiplinger’s Free Newsletters
Profit and prosper with the best of expert advice on investing, taxes, retirement, personal finance and more - straight to your e-mail.
Profit and prosper with the best of expert advice - straight to your e-mail.
Some drugs may be difficult to substitute if you’re in the middle of treatment, says Dan Johnson, of ScriptSave WellRX, which provides price comparisons and a discount card. In that case, your best option may be to work with your doctor to file an appeal with the plan.
Profit and prosper with the best of Kiplinger's advice on investing, taxes, retirement, personal finance and much more. Delivered daily. Enter your email in the box and click Sign Me Up.

As the "Ask Kim" columnist for Kiplinger's Personal Finance, Lankford receives hundreds of personal finance questions from readers every month. She is the author of Rescue Your Financial Life (McGraw-Hill, 2003), The Insurance Maze: How You Can Save Money on Insurance -- and Still Get the Coverage You Need (Kaplan, 2006), Kiplinger's Ask Kim for Money Smart Solutions (Kaplan, 2007) and The Kiplinger/BBB Personal Finance Guide for Military Families. She is frequently featured as a financial expert on television and radio, including NBC's Today Show, CNN, CNBC and National Public Radio.
